What is Ulcer Management?
Ulcer management, particularly in diabetic foot ulcers and venous ulcers, involves a comprehensive approach to wound care aimed at promoting healing, preventing complications, and improving the patient's quality of life. Both diabetic foot ulcers and venous ulcers are chronic wounds that require specialized care due to their complex etiology and potential for complications.
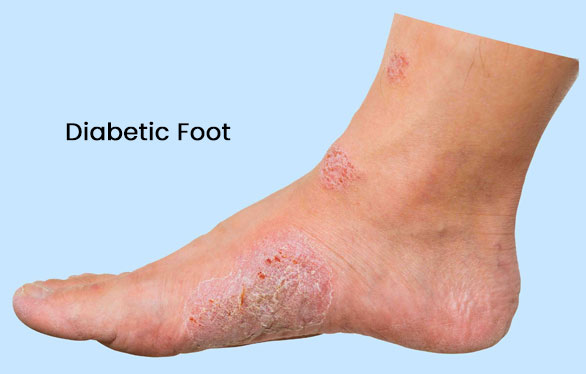
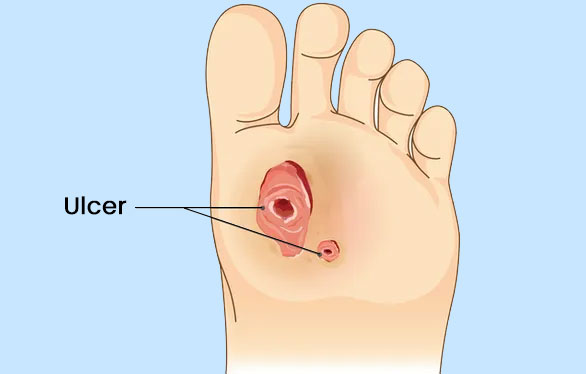
Here's an overview of management strategies for diabetic foot ulcers:
1. Wound Assessment
- Evaluate Wound Characteristics: Assess size, depth, location, and presence of infection.
- Assess Vascular Status: Check for adequate blood flow to the wound site.
- Assess Neuropathy: Evaluate sensory loss and motor function to determine risk of further injury.
2. Offloading
- Pressure Redistribution: Use specialized footwear, casts, or orthotic devices to relieve pressure on the ulcer site.
- Activity Modification: Encourage limited weight-bearing or non-weight-bearing activities to reduce pressure on the foot.
3. Wound Debridement
- Remove Necrotic Tissue: Debride non-viable tissue to promote wound healing.
- Sharp Debridement: Remove necrotic tissue using surgical instruments.
- Enzymatic or Autolytic Debridement: Use topical agents or dressings to facilitate natural tissue breakdown.
4. Infection Management
- Culture and Sensitivity Testing: Obtain wound cultures to identify pathogens and guide antibiotic therapy.
- Systemic Antibiotics: Administer antibiotics for infected ulcers based on culture results and clinical judgment.
- Topical Antimicrobial Agents: Apply topical antimicrobials to reduce bacterial burden in the wound.
5. Moist Wound Healing
- Use Moist Dressings: Apply dressings that maintain a moist wound environment to promote granulation tissue formation and epithelialization.
- Hydrogels, Hydrocolloids, and Foam Dressings: Choose dressings appropriate for the wound characteristics and exudate levels.
6. Vascular Assessment and Intervention
- Vascular Evaluation: Assess vascular status through non-invasive vascular studies (e.g., ankle-brachial index) or imaging (e.g., angiography).
- Revascularization: Consider vascular interventions (angioplasty, stenting, bypass surgery) to improve blood flow to the affected limb if indicated.
7. Patient Education
- Foot Care Education: Teach patients about proper foot hygiene, nail care, and footwear selection to prevent future ulcers.
- Wound Self-management: Instruct patients on wound care techniques, dressing changes, and signs of infection.
8. Multidisciplinary Care
- Collaborative Approach: Involve a multidisciplinary team including podiatrists, wound care specialists, vascular surgeons, endocrinologists, and infectious disease specialists.
- Regular Follow-up: Schedule regular follow-up appointments to monitor wound progress, address complications, and adjust treatment as needed.
Here's an overview of management strategies for venous ulcer:
1. Compression Therapy
- Apply Compression Bandages or Stockings: Promotes venous return, reduces edema, and improves ulcer healing.
- Graduated Compression: Ensure proper compression levels tailored to the patient's needs and tolerance.
2. Wound Debridement
- Remove Necrotic Tissue: Debride non-viable tissue to facilitate wound healing.
- Sharp or Enzymatic Debridement: Use appropriate techniques to remove necrotic tissue while minimizing trauma to the wound bed.
3. Moist Wound Healing
- Use Moist Dressings: Apply dressings that maintain a moist wound environment to promote healing.
- Hydrocolloids, Foam Dressings, Alginate Dressings: Choose dressings based on wound characteristics and exudate levels.
4. Edema Management
- Elevation: Encourage limb elevation to reduce edema and improve venous return.
- Diuretics: Consider diuretic therapy in patients with significant edema.
5. Vascular Assessment
- Evaluate Venous Insufficiency: Assess venous reflux and venous obstruction through clinical evaluation and non-invasive vascular studies.
- Venous Ultrasound: Perform venous duplex ultrasound to identify underlying venous pathology.
6. Lifestyle Modification
- Encourage Physical Activity: Promote regular exercise to improve calf muscle pump function and venous return.
- Weight Management: Advise weight loss in overweight or obese patients to reduce venous hypertension.
7. Nutritional Support
- Ensure Adequate Nutrition: Provide nutritional counseling and supplements as needed to support wound healing.
- Optimize Protein Intake: Ensure sufficient protein intake to promote tissue repair and regeneration.
8. Patient Education
- Compression Therapy Education: Teach patients about proper application and maintenance of compression bandages or stockings.
- Skin Care Education: Instruct patients on skin hygiene, moisturization, and prevention of skin breakdown.
What are the treatment options for Ulcer Management?
1. Endovascular Therapy for Arterial Ulcers
- Angioplasty and Stenting: This procedure involves the use of a balloon catheter to open narrowed or blocked arteries and the placement of a stent to keep the artery open. This improves blood flow to the ulcerated area, promoting healing.
- Atherectomy: This involves the removal of plaque from the arteries using a specialized catheter with a cutting device, laser, or other mechanisms.
2. Embolization for Venous Ulcers
- Varicose Vein Treatment: For venous ulcers caused by chronic venous insufficiency, embolization procedures like sclerotherapy or endovenous laser therapy (EVLT) are used to close off malfunctioning veins.
- Sclerotherapy: A sclerosant solution is injected into the affected veins, causing them to scar and close.
- Endovenous Laser Therapy (EVLT): A laser fiber is inserted into the vein, and laser energy is applied to close the vein.
3. Wound Debridement and Healing
- Ultrasound-Guided Debridement: Use of ultrasound to guide the removal of dead or infected tissue from the ulcer to promote healing.
- Advanced Dressing Application: Application of specialized wound dressings, sometimes under image guidance, to promote a moist wound environment conducive to healing.
4. Hyperbaric Oxygen Therapy (HBOT)
- Procedure: HBOT involves breathing pure oxygen in a pressurized chamber. This treatment increases the amount of oxygen in the blood, enhancing wound healing, particularly for diabetic foot ulcers.
5. Percutaneous Ablation for Venous Insufficiency
- Radiofrequency Ablation (RFA): Use of radiofrequency energy to heat and close off incompetent veins that contribute to venous ulcers.
6. Injection Therapies
- Platelet-Rich Plasma (PRP) Therapy: Injection of concentrated platelets from the patient’s own blood into the ulcer site to promote healing.
7. Laser Therapy for Ulcer Healing
- Low-Level Laser Therapy (LLLT): Application of low-level lasers to the ulcer to promote tissue repair and reduce inflammation.
8. Interventional Procedures for Diabetic Foot Ulcers
- Angioplasty and Stenting: As with arterial ulcers, improving blood flow through angioplasty and stenting can significantly aid in the healing of diabetic foot ulcers.
- Debridement and Infection Control: Using interventional techniques to clean and debride the wound, combined with appropriate antibiotics to manage infections.
9. Vascular Imaging and Assessment
- Doppler Ultrasound and Angiography: Non-invasive imaging techniques to assess blood flow and guide treatment decisions for ulcer management.
Follow-Up and Monitoring
- Regular Follow-Up: Ensuring the ulcer is healing properly and adjusting treatment as necessary.
- Imaging: Periodic imaging to assess the status of blood flow and the effectiveness of treatments.
Benefits of Interventional Radiology in Ulcer Management
- Minimally Invasive: Most procedures are less invasive than traditional surgery, with fewer risks and quicker recovery times.
- Targeted Treatment: Procedures are highly targeted, focusing on the specific area causing the problem.
- Outpatient Basis: Many treatments can be performed on an outpatient basis, reducing hospital stays.
