What is stroke?
A stroke, also known as a cerebrovascular accident (CVA), occurs when the blood supply to part of the brain is interrupted or reduced, preventing brain tissue from getting the necessary oxygen and nutrients. This can result in brain cells beginning to die within minutes. Strokes are a medical emergency that requires immediate attention to minimize brain damage and potential complications.
Types of Stroke
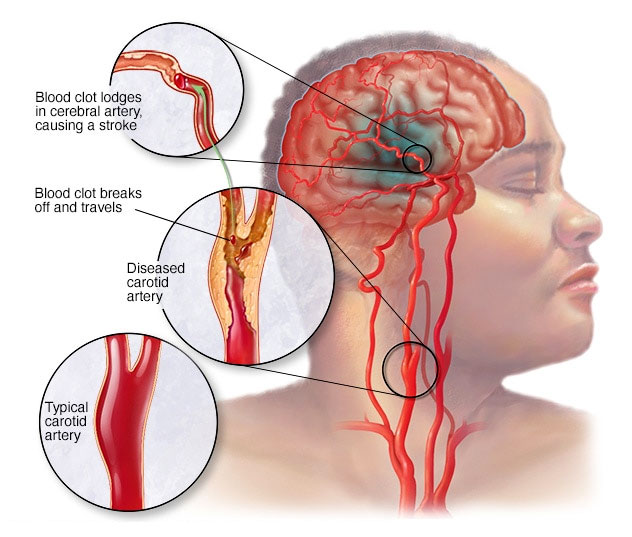
- Ischemic Stroke Ischemic Stroke occur when an artery supplying blood to the brain becomes blocked, usually by a blood clot.
- Hemorrhagic Stroke Hemorrhagic strokes occur when a blood vessel in the brain ruptures, leading to bleeding in or around the brain.
- Transient Ischemic Attack (TIA) A Transient Ischemic Attack (TIA), often called a mini-stroke, is a temporary period of symptoms similar to those of a stroke. A TIA occurs when a blood clot temporarily blocks an artery, causing a short-term disruption in blood flow to part of the brain. TIAs typically last a few minutes to a few hours and do not cause permanent damage. However, they are a significant warning sign of the potential for a future, more severe stroke.
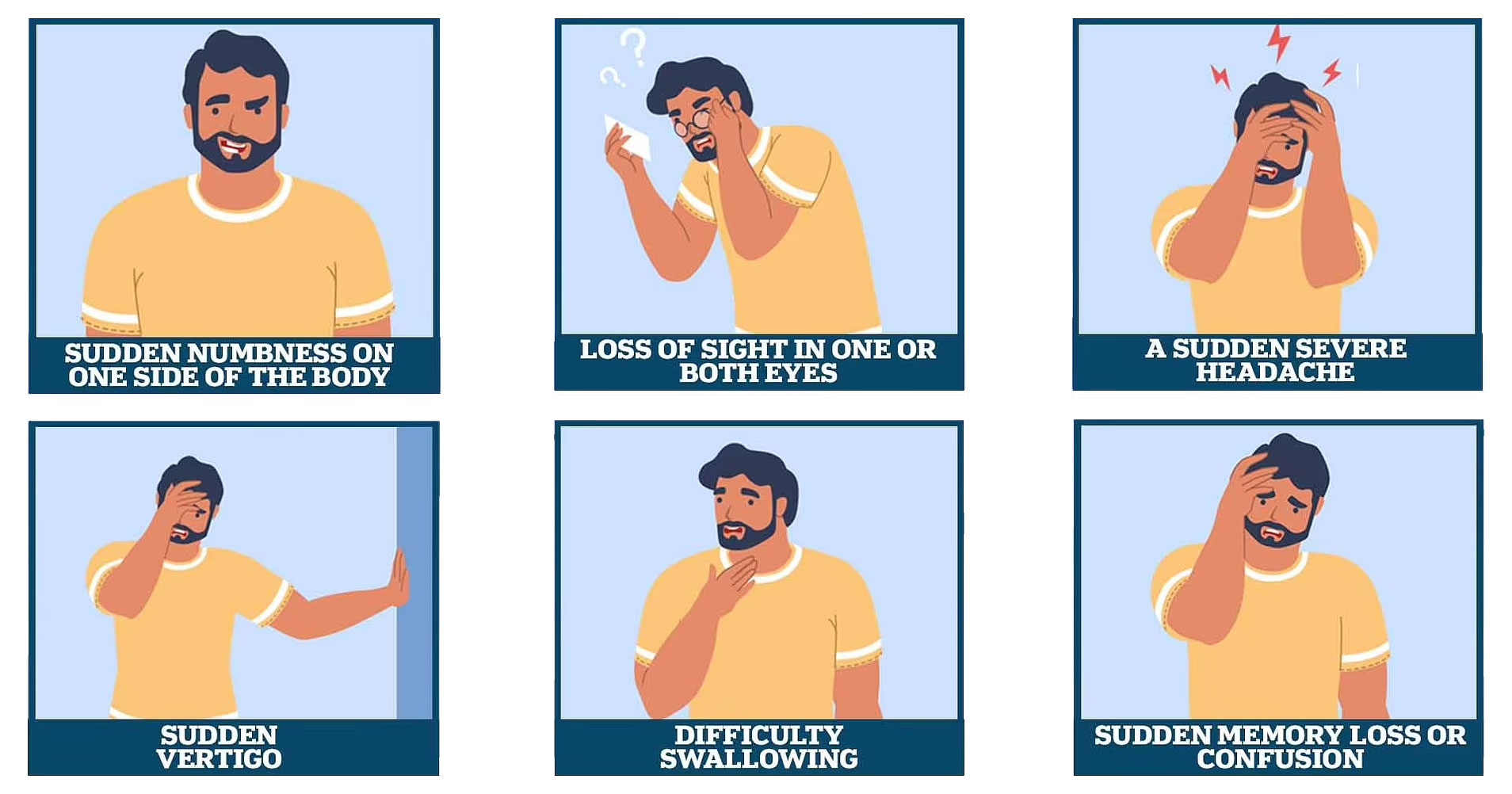
What are the symptoms of stroke?
- Sudden numbness or weakness in the face, arm, or leg, especially on one side of the body.
- Sudden confusion, trouble speaking, or understanding speech.
- Sudden trouble seeing in one or both eyes.
- Sudden trouble walking, dizziness, loss of balance, or coordination.
- Sudden severe headache with no known cause.
What are the risk factors of stroke?
Certain risk factors increase the likelihood of having a stroke, whether ischemic or hemorrhagic. These include:
- High Blood Pressure: The most significant risk factor for both types of stroke.
- Diabetes: Increases the risk of atherosclerosis and clot formation.
- Heart Diseases: Such as coronary artery disease, heart failure, and atrial fibrillation.
- High Cholesterol: Contributes to plaque buildup in arteries.
- Smoking: Damages blood vessels and increases the risk of clot formation.
- Obesity: Associated with high blood pressure, diabetes, and heart disease.
- Physical Inactivity: Contributes to the development of several risk factors.
- Unhealthy Diet: High in saturated fats, trans fats, cholesterol, and sodium.
- Excessive Alcohol Consumption: Can raise blood pressure and contribute to other risk factors.
- Family History: A family history of stroke or TIA increases the risk.
- Age: Risk increases with age, particularly after 55.
- Gender: Men have a higher risk of stroke, but women have a higher risk of mortality from stroke.
- Race and Ethnicity: African Americans have a higher risk of stroke than other racial groups.
Importance of Immediate Medical Attention
Recognizing the symptoms of a stroke and seeking immediate medical attention is crucial. The acronym FAST can help remember the warning signs:
- Face drooping: Does one side of the face droop or is it numb?
- Arm weakness: Is one arm weak or numb?
- Speech difficulty: Is speech slurred, are they unable to speak, or are they hard to understand?
- Time to call emergency services: If someone shows any of these symptoms, even if they go away, call emergency services immediately.
Early treatment can significantly improve outcomes and reduce the risk of severe complications or death.
What are the treatment options for stroke?
Mechanical Thrombectomy
- Indication: Acute ischemic stroke caused by a large vessel occlusion, typically within 6 hours of symptom onset, but can be extended to 24 hours in certain cases.
- Procedure:
- Imaging: Initial brain imaging (CT or MRI) to confirm the diagnosis and location of the clot.
- Access: A catheter is inserted into a blood vessel in the groin or wrist and navigated to the blocked artery in the brain.
- Clot Retrieval: Specialized devices, such as stent retrievers or aspiration catheters, are used to capture and remove the clot.
- Benefits: Can significantly improve outcomes by restoring blood flow, reducing the extent of brain damage, and improving functional recovery.
Intra-Arterial Thrombolysis
- Indication: Acute ischemic stroke, particularly when intravenous thrombolysis (IV tPA) is contraindicated or has not been effective, typically within 6 hours of symptom onset.
- Procedure:
- Imaging: Initial brain imaging to confirm the diagnosis and location of the clot.
- Access: A catheter is inserted into a blood vessel and navigated to the site of the clot.
- Thrombolytic Agent: Direct administration of a thrombolytic drug (e.g., tPA) into the clot to dissolve it.
- Benefits: Targeted delivery of the thrombolytic agent can be more effective in certain cases and reduces systemic exposure to the drug.
Carotid Artery Stenting (CAS)
- Indication: Stroke prevention in patients with significant carotid artery stenosis, particularly for those who are high-risk surgical candidates.
- Procedure:
- Imaging: Duplex ultrasound, CT angiography, or MR angiography to assess the degree of stenosis.
- Access: A catheter is inserted into a blood vessel and navigated to the carotid artery.
- Stenting: A balloon is used to expand the narrowed segment of the artery, followed by the placement of a stent to keep it open.
- Benefits: Minimally invasive alternative to carotid endarterectomy, reduces the risk of stroke in patients with significant carotid artery disease.
Angioplasty
- Indication: Treatment of intracranial or extracranial arterial stenosis contributing to stroke risk.
- Procedure:
- Imaging: Initial imaging to confirm the location and extent of the stenosis.
- Access: A catheter is inserted and navigated to the site of the stenosis.
- Balloon Angioplasty: A balloon is inflated to widen the narrowed artery.
- Benefits: Improves blood flow, reduces stroke risk, and can be combined with stenting for long-term results.
Aneurysm Coiling and Flow Diversion
- Indication: Prevention of stroke due to aneurysmal rupture.
- Procedure:
- Imaging: Detailed imaging to identify aneurysms.
- Access: A catheter is inserted and navigated to the aneurysm.
- Coiling: Coils are deployed into the aneurysm sac to induce clotting and prevent rupture.
- Flow Diversion: Placement of a flow-diverting stent to redirect blood flow away from the aneurysm, promoting healing and reducing rupture risk.
- Benefits: Minimally invasive, reduces the risk of aneurysm rupture and subsequent hemorrhagic stroke.
