What is peripheral vascular disease?
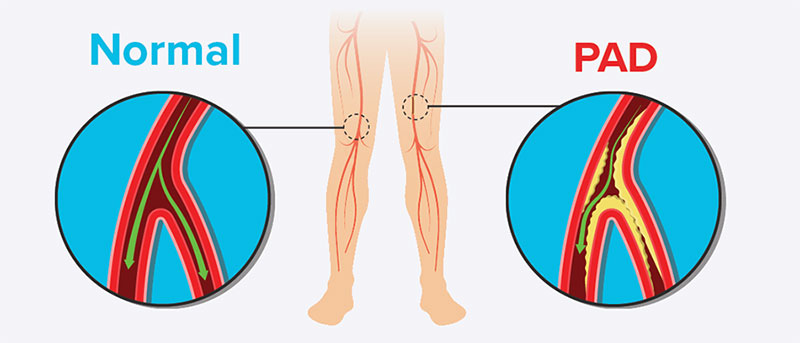
Peripheral vascular disease (PVD), also known as peripheral artery disease (PAD) when specifically referring to arteries, is a condition characterized by the narrowing or blockage of blood vessels outside the heart and brain. This can lead to reduced blood flow, typically to the legs, but can also affect other areas such as the arms, stomach, and kidneys.
What are the symptoms of peripheral vascular disease?
- Intermittent claudication: Pain, cramping, or tiredness in the leg or hip muscles while walking or exercising that goes away with rest.
- Leg numbness or weakness.
- Coldness in the lower leg or foot, especially when compared to the other leg.
- Sores on toes, feet, or legs that won't heal.
- A change in the color of the legs.
- Hair loss or slower hair growth on the feet and legs.
- Slower growth of toenails.
- Shiny skin on the legs.
- Weak pulse in the legs or feet.
What are the causes & risk factors of peripheral vascular disease?
- Atherosclerosis: The most common cause, where fatty deposits build up on the artery walls, reducing blood flow.
- Smoking: A major risk factor that damages the blood vessels.
- Diabetes: Increases the risk of PAD due to the effects on blood vessels and circulation.
- Obesity: Excess weight contributes to atherosclerosis and other conditions that can cause PAD.
- High blood pressure and cholesterol: Contribute to the build-up of plaques in the arteries.
- Age: Risk increases with age, especially over 50.
- Family history: Genetics can play a role in the development of PAD.
- Sedentary lifestyle: Lack of physical activity can increase the risk.
What are the treatment options for peripheral vascular disease?
Here are the main treatment methods:
1. Lifestyle Modifications
- Smoking Cessation: Stopping smoking to improve overall vascular health.
- Exercise: Regular physical activity, particularly walking, to improve circulation and reduce symptoms.
- Diet: A heart-healthy diet low in saturated fats, cholesterol, and sodium to manage weight and improve blood flow.
- Weight Management: Maintaining a healthy weight to reduce strain on the vascular system.
2. Medications
- Antiplatelet Agents: Drugs like aspirin or clopidogrel to reduce blood clotting and improve blood flow.
- Statins: Cholesterol-lowering medications to slow the progression of atherosclerosis
- Antihypertensives: Medications to control high blood pressure.
- Cilostazol: A medication to improve symptoms of claudication (pain caused by too little blood flow during exercise).
3. Endovascular Procedures
- Angioplasty: A catheter with a balloon at its tip is inserted into the narrowed artery. The balloon is inflated to open up the artery and improve blood flow.
- Stenting: Often performed with angioplasty, a small wire mesh tube (stent) is inserted into the artery to keep it open.
- Atherectomy: A procedure to remove plaque from the artery using a catheter with a cutting device at its tip.
4. Surgical Procedures
- Bypass Surgery: Creating a bypass around the blocked artery using a vessel from another part of the body or a synthetic graft to restore blood flow.
- Endarterectomy: Surgical removal of plaque from the inner lining of the artery.
5. Thrombolytic Therapy
- Catheter-Directed Thrombolysis: A catheter is used to deliver clot-dissolving medication directly to the site of a blood clot in the artery.
6. Non-Surgical Interventions
- Percutaneous Transluminal Angioplasty (PTA): Similar to angioplasty, PTA is a minimally invasive procedure to widen the narrowed arteries using a balloon catheter.
7. Compression Therapy
- Compression Stockings: To help manage symptoms like swelling and improve circulation, particularly in veins.
8. Symptom Management and Pain Relief
- Pain Medications: To manage pain associated with PVD.
- Physical Therapy: Programs to help improve mobility and reduce symptoms.
9. Monitoring and Follow-Up
- Regular Check-Ups: Routine monitoring to assess the progression of the disease and effectiveness of treatments.
- Imaging Studies: Ultrasound, MRI, or CT angiography to evaluate blood flow and detect any new blockages.
10. Patient Education
- Risk Factor Management: Education on controlling risk factors such as diabetes, high blood pressure, and high cholesterol.
- Self-Care Techniques: Instructions on foot care and recognizing symptoms that require immediate medical attention.
How to prevent peripheral vascular disease?
- Stop smoking: One of the most effective ways to reduce risk.
- Exercise regularly: Helps improve circulation and overall cardiovascular health.
- Healthy diet: Low in saturated fats, trans fats, and cholesterol.
- Manage chronic conditions: Keep diabetes, high blood pressure, and cholesterol under control.
- Regular check-ups: Monitoring and managing risk factors with a healthcare provider.
